Rheumatoid Arthritis
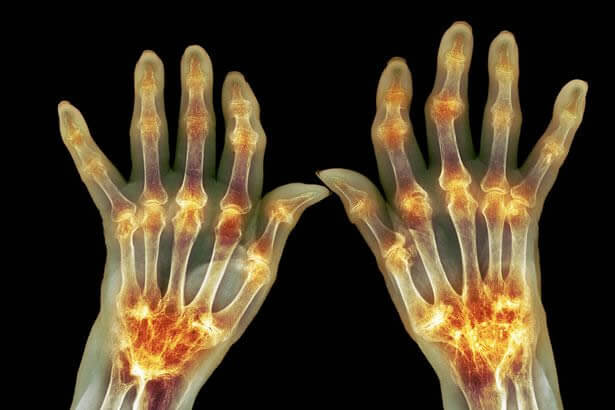 Rheumatoid arthritis is a chronic inflammatory disorder that can affect more than just your joints. In some people, the condition can damage a wide variety of body systems, including the skin, eyes, lungs, heart and blood vessels.
Rheumatoid arthritis is a chronic inflammatory disorder that can affect more than just your joints. In some people, the condition can damage a wide variety of body systems, including the skin, eyes, lungs, heart and blood vessels.
An autoimmune disorder, rheumatoid arthritis occurs when your immune system mistakenly attacks your own body’s tissues.
Unlike the wear-and-tear damage of osteoarthritis, rheumatoid arthritis affects the lining of your joints, causing a painful swelling that can eventually result in bone erosion and joint deformity.
The inflammation associated with rheumatoid arthritis is what can damage other parts of the body as well.
Symptoms for Rheumatoid Arthritis
Signs and symptoms of rheumatoid arthritis may include:
- Tender, warm, swollen joints
- Joint stiffness that is usually worse in the mornings and after inactivity
- Fatigue, fever and loss of appetite
Early rheumatoid arthritis tends to affect your smaller joints first — particularly the joints that attach your fingers to your hands and your toes to your feet.
As the disease progresses, symptoms often spread to the wrists, knees, ankles, elbows, hips and shoulders. In most cases, symptoms occur in the same joints on both sides of your body.
About 40 percent of the people who have rheumatoid arthritis also experience signs and symptoms that don’t involve the joints. Rheumatoid arthritis can affect many nonjoint structures such as eyes, nerve issue, etc.
Rheumatoid arthritis signs and symptoms may vary in severity and may even come and go. Over time, rheumatoid arthritis can cause joints to deform and shift out of place.
Causes for Rheumatoid Arthritis
Rheumatoid arthritis occurs when your immune system attacks the synovium — the lining of the membranes that surround your joints.
Doctors don’t know what starts this process, although a genetic component appears likely. While your genes don’t actually cause rheumatoid arthritis, they can make you more susceptible to environmental factors — such as infection with certain viruses and bacteria — that may trigger the disease.
Diagnosis for Rheumatoid Arthritis
During the physical exam, your doctor will check your joints for swelling, redness and warmth. He or she may also check your reflexes and muscle strength.
Blood tests for Rheumatoid Arthritis
People with rheumatoid arthritis often have an elevated erythrocyte sedimentation rate (ESR, or sed rate) or C-reactive protein (CRP), which may indicate the presence of an inflammatory process in the body. Other common blood tests look for rheumatoid factor and anti-cyclic citrullinated peptide (anti-CCP) antibodies.
Imaging tests for Rheumatoid Arthritis
Your doctor may recommend X-rays to help track the progression of rheumatoid arthritis in your joints over time. MRI and ultrasound tests can help your doctor judge the severity of the disease in your body.
Treatment for Rheumatoid Arthritis
There is no cure for rheumatoid arthritis. But clinical studies indicate that remission of symptoms is more likely when treatment begins early with medications known as disease-modifying antirheumatic drugs (DMARDs).
Medications for Rheumatoid Arthritis
The types of medications recommended by your doctor will depend on the severity of your symptoms and how long you’ve had rheumatoid arthritis
- NSAIDs. Nonsteroidal anti-inflammatory drugs (NSAIDs) can relieve pain and reduce inflammation. Over-the-counter NSAIDs include ibuprofen (Advil, Motrin IB) and naproxen sodium (Aleve). Stronger NSAIDs are available by prescription. Side effects may include stomach irritation, heart problems and kidney damage.
- Steroids. Corticosteroid medications, such as prednisone, reduce inflammation and pain and slow joint damage. Side effects may include thinning of bones, weight gain and diabetes. Doctors often prescribe a corticosteroid to relieve acute symptoms, with the goal of gradually tapering off the medication.
- Disease-modifying antirheumatic drugs (DMARDs). These drugs can slow the progression of rheumatoid arthritis and save the joints and other tissues from permanent damage. Common DMARDs include Methotrexate, leflunomide , hydroxychloroquine and sulfasalazine
Side effects vary but may include liver damage, bone marrow suppression and severe lung infections.
- Biologic agents. Also known as biologic response modifiers
These drugs can target parts of the immune system that trigger inflammation that causes joint and tissue damage. These types of drugs also increase the risk of infections. Biologic DMARDs are usually most effective when paired with a nonbiologic DMARD, such as methotrexate.
Questions? Call us at 703-734-2222 during business hours.
Arthritis & Rheumatology Clinical Center of Northern Virginia has been providing the best rheumatologic care to patients throughout Northern Virginia. Our doctors are board certified in rheumatology.